Health
AU Endorses Initiatives to End AIDS by 2030


By Dipo Olowookere
African heads of state have endorsed two major new initiatives to help end AIDS by 2030. The community health workers initiative aims to recruit, train and deploy 2 million community health workers across Africa by 2020.
The western and central Africa catch-up plan aims to rapidly accelerate access to HIV treatment in the region and close the gap in access between African regions. The initiatives were endorsed at the AIDS Watch Africa Heads of State and Government Meeting, held on 3 July during the 29th African Union Summit in Addis Ababa, Ethiopia.
Western and central Africa catch-up plan
Under the leadership of countries and regional economic communities, and in collaboration with UNAIDS, the World Health Organization, Doctors Without Borders and other partners, the catch-up plan in western and central Africa, which started implementation in late 2016, seeks to dramatically accelerate the scale-up of HIV testing, prevention and treatment programmes, with the goal of putting the region on the Fast-Track to meet the 90–90–90 targets by December 2020.
While the world witnesses significant progress in responding to HIV, with 57% of all people living with HIV knowing their HIV status, 46% of all people living with HIV accessing treatment and 38% of all people living with HIV virally suppressed in 2015, the western and central Africa region lags behind, achieving only 36%, 28% and 12%, respectively, in 2015. The gap is considerable: 4.7 million people living with HIV are not receiving treatment, and 330 000 adults and children died from AIDS-related illnesses in 2015.
“We cannot accept a two-speed approach to ending AIDS in Africa,” said UNAIDS Executive Director Michel Sidibé. “To put western and central Africa on track to end AIDS, we must address stigma, discrimination and other challenges to an effective response, allocate funding to support the most effective strategies and implement delivery strategies that reach the communities most in need.”
The catch-up plan will aim to increase the number of people on treatment from 1.8 million to 2.9 million by mid-2018, giving an additional 1.2 million people, including 120 000 children, access to urgently needed treatment.
The first call for a catch-up plan for the region was made at the United Nations General Assembly High-Level Meeting on Ending AIDS in June 2016. Since then, at least 10 countries (Benin, Cameroon, the Central African Republic, Côte d’Ivoire, the Democratic Republic of the Congo, Guinea, Liberia, Nigeria, Senegal and Sierra Leone) have developed country operational plans deriving from the western and central Africa catch-up plan with a focus on ensuring the needed policy and structural changes.
Two million community health workers
The community health worker initiative aims to accelerate progress towards achieving the 90–90–90 targets by 2020—whereby 90% of all people living with HIV know their HIV status, 90% of people who know their HIV-positive status are accessing treatment and 90% of people on treatment have suppressed viral loads—and to lay the foundation for sustainable health systems. Championed by the President of Guinea and African Union Chair, Alpha Condé, the initiative seeks to confront the acute health workforce shortages across Africa and improve access to health services for the most marginalized populations, including people living in rural areas.
“Recruiting 2 million community health workers is a critical step towards achievement of the Africa-wide socioeconomic transformation envisioned in the African Union’s Agenda 63”, said Mr Condé. “Few tools have the ability of community health workers to drive progress across the entire breadth of the 2030 Agenda for Sustainable Development.”
Substantial evidence, from both Africa and elsewhere, demonstrates that well-trained, properly supervised community health workers provide an excellent quality of care and improve the efficiency and impact of health spending. Community health workers have helped devise some of the most effective service delivery strategies for HIV testing and treatment, and studies have also linked community-delivered services with increased rates of immunization, exclusive breastfeeding and malaria control coverage.
“Sustainable community health work is a matter of survival and development in Ethiopia, said Prime Minister of Ethiopia Hailemariam Desalegn. “My community health workers have made better health happen. Achieving universal health coverage is not possible without building community health systems.”
UNAIDS estimates that there are more than 1 million community health workers in Africa today, but most focus on a single health problem and are under-trained, unpaid or under-paid, and not well integrated in health systems. The new initiative endorsed by AIDS Watch Africa seeks to retrain existing community health workers, where feasible, and to recruit new health workers to reach the 2 million target.
“Few investments generate such a remarkable social and economic return as community health workers,” said Jeffrey Sachs, Director, Earth Institute, Columbia University. “Community health worker programmes are essentially self-sustaining, in that they avert illness, keep workers healthy and productive and contribute to economic growth and opportunity.”
While community health workers may hold the key in many settings to achieving the 90–90–90 targets, the benefits of this new initiative extend well beyond the AIDS response. The initiative will expedite gains across the health targets of Sustainable Development Goal 3, create new jobs that will strengthen local and national economies and offer new opportunities to young people. The new initiative is aligned with the World Health Organization’s Global Strategy on Human Resources for Health.
Start Free Stay Free AIDS Free
At the AIDS Watch Africa meeting, the participants also called on member states and development partners to support the African Union campaign to eliminate new HIV infections among children and keep mothers alive as part of the Start Free Stay Free AIDS Free collaborative framework.
“Complacency gives birth to regression of the gains made in reducing HIV prevalence, said, Yoweri Museveni, President of Uganda. “We in Uganda have rekindled the campaign to end AIDS; the science exists, as well as the medication. We can win this battle.”
Health
Nigeria on High Alert as WHO Declares Ebola Emergency of International Concern
By Adedapo Adesanya
The Nigeria Centre for Disease Control and Prevention (NCDC) has said that although the country currently has no confirmed case of Ebola Virus Disease (EVD), it is, nevertheless, actively strengthening surveillance.
This comes as the World Health Organisation (WHO) declared the Ebola outbreak in Congo and Uganda a public health emergency of international concern, after 80 deaths were attributed to the disease.
The WHO, however, stopped short of declaring a pandemic, saying it did not meet the necessary criteria. The United Nations agency advised countries against closing borders or restricting trade.
Early symptoms include fever, muscle pain, fatigue, headache, and sore throat, and are followed by vomiting, diarrhoea, a rash, and bleeding.
In a statement by its Director General, Mr Jide Idris, on Sunday, the NCDC noted that it is also ramping up laboratory readiness, infection prevention, and public awareness efforts across the country.
He said the centre was closely monitoring the situation due to increasing regional movement across African countries and was working with relevant stakeholders, including the Port Health Services under the Federal Ministry of Health and Social Welfare, to strengthen preparedness within Nigeria’s public health system.
“NCDC is closely monitoring the situation and working with relevant stakeholders, including the Port Health Services, to ensure continued vigilance and preparedness within the public health system,” he stated.
The NCDC boss described Ebola virus disease as a severe viral illness transmitted through direct contact with the blood, bodily fluids, secretions, or contaminated materials of infected persons or animals.
He noted that the disease has an incubation period ranging from two to 21 days, while symptoms include fever, weakness, headache, muscle pain, sore throat, vomiting, diarrhoea, and, in severe cases, unexplained bleeding.
Recall that Nigeria gained international recognition for successfully containing an Ebola outbreak in 2014 after an infected traveller arrived in Lagos from Liberia.
Healthcare workers were advised to maintain a high index of suspicion for Ebola, especially in patients presenting symptoms compatible with the disease alongside relevant travel or exposure history.
Idris stressed the importance of strict adherence to infection prevention and control measures, including early identification and isolation of suspected cases, proper use of personal protective equipment, hand hygiene, and prompt reporting through established channels.
“NCDC will continue to monitor the situation closely and provide updates as necessary,” he added.
NCDC advised Nigerians to remain calm, maintain good hand hygiene, avoid misinformation, and report unusual illnesses promptly.
Health
NNPC Donates MRI Machine, Others to Nnewi Teaching Hospital
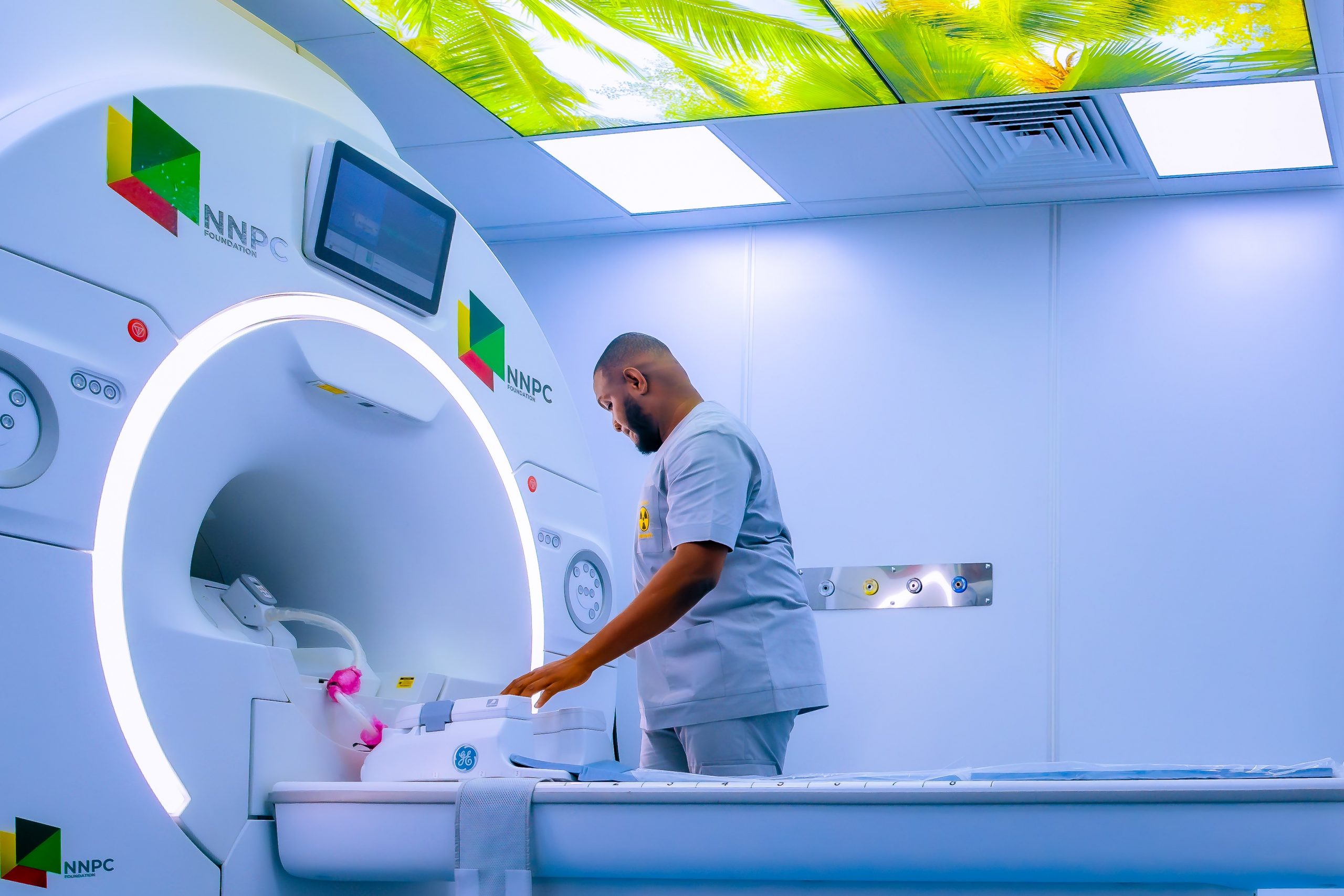
By Modupe Gbadeyanka
A 1.5 Tesla Magnetic Resonance Imaging (MRI) machine has been donated to the Nnamdi Azikiwe University Teaching Hospital (NAUTH), Nnewi, Anambra State, by the corporate social responsibility arm of the Nigerian National Petroleum Company (NNPC) Limited, NNPC Foundation.
In a statement on Sunday by its Chief Corporate Communications Officer, Mr Andy Odeh, the state-owned oil organisation said the medical item was given to the healthcare institution as part of its commitment to improving healthcare access and strengthening medical infrastructure across Nigeria.
The MRI system is expected to significantly improve access to advanced diagnostic imaging services for millions of Nigerians across the South-East (Anambra, Enugu, Imo, Abia and Ebonyi States) as well as neighbouring Delta State.
The foundation also provided critical supporting infrastructure, including RF shielding systems, chillers, backup UPS systems, electrical installations, specialised imaging accessories, ventilation systems, CCTV and oxygen monitoring systems, intercom communication facilities, and other patient comfort technologies designed to ensure optimal operation of the facility.
Before now, patients requiring advanced MRI diagnostic services often faced prolonged waiting periods, exorbitant costs, and the burden of travelling long distances in search of functional imaging centres.
But it is believed that the intervention of the NNPC Foundation would provide succour to patients.
At the presentation of the items to the institution over the weekend, the chief executive of the NNPC, Mr Bashir Bayo Ojulari, represented by the Managing Director of NNPC Foundation, Mrs Emmanuella Arukwe, described the intervention as a strategic investment in healthcare access, diagnostic precision, and improved patient outcomes, noting that the facility aligns with the company’s commitment to building sustainable systems and impactful national institutions.
“The installation of the MRI in NAUTH exemplifies our commitment, as our intent is to build enduring institutions, sustainable systems and legacies. This intervention aligns with our conviction that access to quality healthcare underpins human dignity, longevity and economic productivity,” Mr Ojulari stated.
He described the company’s social investments as viable currencies that strengthen the relationship between the Company’s core mandate of providing and managing energy for Nigerians and meeting stakeholders’ expectations.
In his remarks, the Governor of Anambra State, Mr Charles Soludo, who was represented by the Commissioner for Health, Dr Afam Obidike, said the intervention would enhance safe and precise diagnosis and treatment for patients across the South-East region.
He also commended NNPC Foundation for donating the MRI facility to the state, noting that the intervention would significantly improve access to quality healthcare services for the people.
The Chief Medical Director of NAUTH, Prof Joseph Ugboaja, thanked the donor for the items, saying NNPC Foundation has demonstrated that corporate social responsibility is not just a policy statement but a lifeline for institutions like ours.
“For too long, patients in our catchment area have had to travel long distances to access this level of diagnostic precision, often at prohibitive costs. With this installation, we will eliminate that burden,” he enthused.
Health
Nigeria Launch €4.2m Initiative to Boost Capacity Against Outbreaks

By Adedapo Adesanya
Nigeria has launched a €4.2 million programme supported by the European Union (EU) and implemented by the World Health Organisation (WHO) to strengthen the country’s capacity to detect and respond to disease outbreaks.
The initiative, known as the EU Support to Public Health Institutes in Nigeria (EU SPIN), will be carried out over four years in partnership with the Federal Ministry of Health and Social Welfare.
It is aimed at improving the performance of selected public health institutions through better coordination, faster information sharing and enhanced workforce capacity.
Speaking at the launch in Abuja on Monday, the Minister of State for Health and Social Welfare, Mr Iziaq Adekunle Salako, described the programme as a significant step towards strengthening Nigeria’s healthcare system.
“This initiative is designed to strengthen our health institutions, and it is truly a welcome development. It will improve the well-being of Nigerians, especially our vulnerable populations,” he said, noting that it aligns with the federal government’s broader health reform agenda.
Nigeria continues to face a dual health burden, with recurring infectious disease outbreaks alongside a growing prevalence of non-communicable diseases such as hypertension and diabetes.
According to the WHO, non-communicable diseases now account for 27 per cent of deaths in the country, while malaria alone contributes about 30 per cent of global malaria fatalities.
Recurrent outbreaks of cholera, diphtheria, Lassa fever, meningitis and Mpox also remain a major public health concern.
The EU SPIN programme is expected to address systemic gaps that slow outbreak response by strengthening collaboration among public health institutions and clarifying roles across federal, state and local levels.
It will also support real-time data systems to enable quicker and more informed decision-making during health emergencies.
A key component of the initiative is workforce development, with plans to train up to 75 per cent of public health staff in leadership, prevention and response strategies, as well as digital skills.
The European Union Ambassador to Nigeria, Mr Gautier Mignon, said the programme reflects a shared commitment to building resilient health systems.
“Through EU SPIN, the European Union is investing in strong, digitally enabled public health institutions in Nigeria. This partnership underscores our commitment to health security and sustainable systems strengthening,” he said.
Also speaking, the WHO Representative in Nigeria, Mr Pavel Ursu, noted that improved coordination and digital tools would enhance the country’s ability to protect lives.
“By improving coordination, skills and digital tools, the project will help protect lives and keep communities healthier,” he said.
Officials said the programme would ultimately strengthen links between public health systems and primary healthcare services, ensuring that communities benefit from faster and more effective responses to health threats.
By 2028, the initiative is expected to deliver more efficient inter-agency coordination, clearer institutional responsibilities and more reliable public health data nationwide, with progress tracked through national monitoring systems and periodic reviews involving government and development partners.
-

 Feature/OPED6 years ago
Feature/OPED6 years agoDavos was Different this year
-
Travel/Tourism10 years ago
Lagos Seals Western Lodge Hotel In Ikorodu
-

 Showbiz3 years ago
Showbiz3 years agoEstranged Lover Releases Videos of Empress Njamah Bathing
-

 Banking8 years ago
Banking8 years agoSort Codes of GTBank Branches in Nigeria
-

 Economy3 years ago
Economy3 years agoSubsidy Removal: CNG at N130 Per Litre Cheaper Than Petrol—IPMAN
-

 Banking3 years ago
Banking3 years agoSort Codes of UBA Branches in Nigeria
-

 Banking3 years ago
Banking3 years agoFirst Bank Announces Planned Downtime
-

 Sports3 years ago
Sports3 years agoHighest Paid Nigerian Footballer – How Much Do Nigerian Footballers Earn



2 Comments