Health
Omose Tasks Governments to Adopt Innovative Primary Healthcare Delivery Model

By Dipo Olowookere
African governments have been charged to adopt “a more innovative model of primary health delivery with grassroots-focused universal health coverage structure that is customised to suit the peculiarities” of the continent.
This advice was given by the Chairman and chief executive of Elkris Group, Dr Elliott Scott Omose, during a media chat with newsmen over the weekend.
The healthcare practitioner, who described primary healthcare in Africa as non-existent, said the continent has the capacity to deliver quality service to its citizens.
Mr Omose is also the founder of PreDiagnosis International, an innovative public healthcare management non-profit organisation with footholds in Nigeria, Sierra Leone, Gambia and a few other African countries.
He pointed out that public healthcare management in most African countries remained poor and ineffective due to the faulty service delivery model and structure that governments and decision-makers adopt.
He emphasised that if the poor and vulnerable population on the continent are enjoying public healthcare, the current structural loophole with universal health coverage in Africa with the glaring absence of Basic, Accessible and Affordable (BAA) healthcare at the primary level must be fixed.
“The United Nations General Assembly High-Level Meeting on Universal Health Coverage in 2019 strongly restated that health is a precondition, outcome and indicator for social, economic and environmental dimensions of UN’s 2030 sustainable development goal,” he reminded African leaders.
“In Africa today, primary healthcare is non-existent as soon as you start to move away from the capital cities because research across the continent reveals an unhealthy pattern whereby pharmacies and local drug stores have been adopted as grassroots (primary) healthcare point by close to 70% of the vulnerable population in the continent.
“In rural Africa, a patient may never get to see or sit before a doctor more than five times in his or her lifetime. And that is usually a result of some intervention outreach by an NGO. For the rest of their lives, they are left at the mercy of pharmacy attendants and quacks as the only alternative to a GP,” he noted.
Continuing, Mr Omose also stated that, “Across the continent, the general hospitals and teaching hospitals are continually overwhelmed because most of the available qualified doctors are concentrated in urban cities and towns while the rural areas have next to nothing, thereby leaving room for self-medication and also for quacks and other unqualified hands to tend citizens’ health needs in the rural, hard to reach areas.
“So, most public health centres, especially in rural areas, rot away due to lack of capable personnel to man them.
“Moreover, before the vulnerable class make it to those facilities because of the huge infrastructure deficit, the majority of their cases are already beyond help.”
“There is an urgent need to embrace a more innovative model of primary health delivery with grassroots-focused universal health coverage structure that is customized to suit the peculiarities of the African terrain.
“Only this way can we begin to show seriousness in the attempt to try to bridge the terribly widening gap between the teaming vulnerable population and access to affordable basic (primary) healthcare,” he stated.
Restating his readiness to assist, Dr Omose submitted that PDI has developed and put to work a workable model for essential health services which offers subsidized, affordable and accessible basic universal health coverage for rural and hard-to-reach areas of Africa.
“As part of our contributions to help our continent overcome this unacceptable situation we find ourselves currently, in 2020, we introduced, in Nigeria, the PDI Basic Universal Healthcare model, which has the PDI 25-point Early Detection System as its strategic core.
“Early this year, we also introduced in Sierra Leone the PDI blue-print for a nationwide Basic (Primary) Healthcare Initiative which goes under the name of Community Basic (Primary) Healthcare Clinic– CBHC.
“For the first time, the PDI Basic Universal Healthcare Model guarantees that the vulnerable African population can have full access to proper one-on-one doctor consultation services by way of a hybrid platform that ensures doctor’s appointment, twenty-four-seven doctor hotline, community mobile clinic, community health hub, free prescription services and other services all year round, twenty-four-seven, all for less than $15 a month, which is less than 30 per cent of the actual cost for the concierge personal health management services.
“We are, therefore, showing that with considerably very little financial outlay, Africa could do a lot more in managing the day-to-day personal basic healthcare needs of the vulnerable population,” he submitted.
Health
NARD Suspends Indefinite Strike, Gives FG Fresh Two-Week Ultimatum

By Adedapo Adesanya
The Nigerian Association of Resident Doctors (NARD) has suspended its planned nationwide indefinite strike, granting the federal government a two-week ultimatum to address lingering welfare issues affecting resident doctors across the country.
The decision was taken after an emergency meeting of the association’s National Executive Council on Tuesday, where members reviewed assurances from government representatives and resolved to give dialogue another chance.
NARD said the suspension was informed by “progress made” in negotiations, particularly commitments on the prompt payment of salary arrears, hazard allowances, and steps toward resolving issues surrounding the Medical Residency Training Fund.
The association did not declare a full resolution of the dispute. It noted that the government had shown “renewed willingness” to address the concerns that triggered the strike threat.
The association noted that while these engagements signalled a willingness by the government to resolve the dispute, several critical issues remain outstanding, particularly the delayed payment of promotion arrears, salary arrears, the 2026 Medical Residency Training Fund (MRTF), and the backlog of 19 months’ professional allowance arrears owed to resident doctors.
It also expressed concern over the Federal Government’s decision to halt the implementation of the reviewed PAT, which had earlier triggered widespread dissatisfaction among its members and raised fears of disruption to healthcare services nationwide.
Despite these unresolved issues, NARD said it opted to suspend the strike as a demonstration of goodwill and commitment to ongoing dialogue, while giving the government a two-week window to take concrete, measurable and verifiable steps to meet its demands.
The association insisted on the immediate reversal of the decision affecting the PAT, payment of all outstanding arrears, prompt disbursement of the MRTF, and full settlement of the accumulated professional allowance backlog.
It warned that it would reconvene at the expiration of the ultimatum to assess the level of compliance and determine its next course of action, adding that failure by the government to meet its demands within the stipulated timeframe would result in the resumption of the suspended strike without further notice.
NARD also called on its members nationwide to remain calm, united and resolute, while urging the Federal Government to act swiftly to prevent a potential crisis in the health sector.
The association further appreciated the interventions of the Vice President and other stakeholders, expressing hope that their involvement would lead to the timely resolution of the dispute and help sustain healthcare delivery across the country.
Health
Jacaranda Gets Funds to Expand Affordable Maternal Healthcare in Kenya

By Modupe Gbadeyanka
To expand affordable healthcare in Kenya, Swedfund has invested about $600,000 into Jacaranda Health Limited (Jacaranda Maternity) to support innovations in neonatal intensive care and strengthen Jacaranda’s ability to provide life-saving services to underserved populations.
Jacaranda Maternity provides high-quality maternal health care at more affordable pricing than typical private providers, focusing on women in Nairobi’s low- and middle-income communities.
The new funding will support the opening of new hospitals, upgrading of neonatal care, and improvements to existing facilities.
Maternal and newborn health outcomes in Kenya remain a challenge, with maternal mortality still high despite improvements in skilled birth attendance.
Public health facilities play a central role but face capacity constraints, while access to reliable, quality care varies across regions and income groups.
Private healthcare providers offering essential maternity services at accessible price points can complement public provision.
Jacaranda Maternity aims to expand its network to six hospitals to achieve financial sustainability while scaling its impact. The healthcare provider is a recognised leader in promoting women’s health, with 71 percent of its staff being women, and a track record of effective environmental and social management.
“This investment will help Jacaranda Maternity provide life-saving care to more women and families while furthering Swedfund’s mission to promote inclusive and sustainable healthcare,” a Senior Investment Manager at Swedfund, Audrey Obara, said.
Health
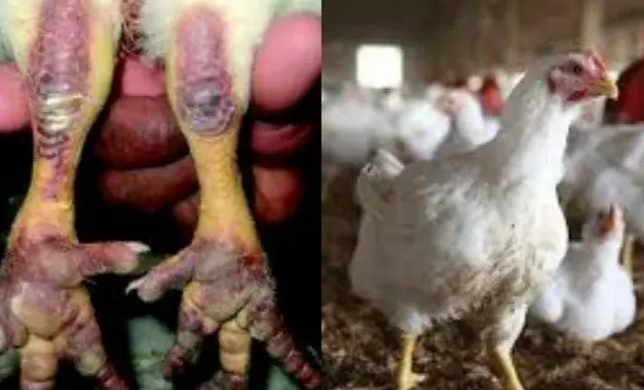
Nigeria Secures $350,000 FAO Support to Tackle Rising Bird Flu
By Adedapo Adesanya
Nigeria will get a $350,000 intervention from the Food and Agriculture Organisation of the United Nations (FAO) to support its response to the ongoing outbreak of Highly Pathogenic Avian Influenza (bird flu) and strengthen the country’s animal health systems.
An agreement was reached on Wednesday during a strategic meeting between the Minister of Livestock Development, Mr Idi Mukhtar Maiha, and the FAO Representative to Nigeria and the Economic Community of West African States, Mr Hussein Gadain, in Abuja.
The intervention, approved under FAO’s Technical Cooperation Programme, will support disease containment efforts in 11 affected states and enhance surveillance, coordination and response mechanisms to prevent further spread of the disease.
Speaking during the meeting, Maiha said effective disease control remains critical to improving livestock productivity and protecting the livelihoods of farmers across the country.
He explained that factors such as drought, scarcity of feed, interaction between livestock and wildlife, as well as cross-border movement of animals have contributed to the spread of diseases in some areas.
“We must continue to strengthen our animal health systems and build the capacity required to respond effectively to disease outbreaks. Our collaboration with FAO will help protect livestock assets, improve productivity and support the broader transformation of the sector,” the minister said.
Mr Gadain commended the federal government’s commitment to the development of the livestock sector and assured that FAO would continue to provide technical support to Nigeria.
He stressed the need to strengthen veterinary services at the state and community levels, improve early detection of diseases and promote biosecurity practices among livestock farmers.
The meeting also reviewed progress on the global campaign to eradicate Peste des Petits Ruminants, a highly contagious disease that affects sheep and goats.
To advance the initiative, the ministry plans to convene a national technical meeting involving veterinary institutions, researchers and practitioners to review Nigeria’s eradication strategy and address gaps in vaccine supply.
As part of preparations, the ministry will engage the National Veterinary Research Institute to assess its vaccine production capacity while exploring other options for vaccine procurement to meet national demand.
Both parties also agreed to accelerate Nigeria’s access to financing under the Pandemic Fund through the One Health approach in collaboration with the Nigeria Centre for Disease Control and the Federal Ministry of Health to strengthen preparedness and response to zoonotic diseases.
Plans are also underway for the Director-General of FAO to participate in the Antimicrobial Resistance Conference scheduled for June 2026 in Abuja, where President Bola Tinubu is expected to be recognised as the African Champion for the eradication of Peste des Petits Ruminants.
The meeting further agreed to inaugurate a Livestock Donor Working Group to coordinate development partner support and advance key initiatives, including the development of a national feed and fodder strategy aimed at improving productivity and sustainability in the livestock sector.
-

 Feature/OPED6 years ago
Feature/OPED6 years agoDavos was Different this year
-
Travel/Tourism10 years ago
Lagos Seals Western Lodge Hotel In Ikorodu
-

 Showbiz3 years ago
Showbiz3 years agoEstranged Lover Releases Videos of Empress Njamah Bathing
-

 Banking8 years ago
Banking8 years agoSort Codes of GTBank Branches in Nigeria
-

 Economy3 years ago
Economy3 years agoSubsidy Removal: CNG at N130 Per Litre Cheaper Than Petrol—IPMAN
-

 Banking3 years ago
Banking3 years agoSort Codes of UBA Branches in Nigeria
-

 Banking3 years ago
Banking3 years agoFirst Bank Announces Planned Downtime
-

 Sports3 years ago
Sports3 years agoHighest Paid Nigerian Footballer – How Much Do Nigerian Footballers Earn

