Health
COVID-19: Urgent Need for African Governments to Upgrade Health Systems
By Kester Kenn Klomegah
Amid multifold theories and disinformation spreading around the COVID-19 in Africa, it is important for African governments to consider strengthening the existing health systems and infrastructures, and allocate substantial funds for health research and production of basic equipment, for attaining sustainable development goals set in the African Agenda 2063, according to experts.
Over the years, most African countries with the exception of South Africa, Botswana and a few others have not improved much on their healthcare system since independence, partly as a result of pure negligence on the part of senior officials who prefer to be treated abroad. The leaders of Cameroon, Nigeria and Zimbabwe are notorious for spending long periods of time abroad in hospitals, according to Dr Chipo Dendere, Zimbabwean Professor of African Politics at Wellesley College in Massachusetts.
As Dendere further noted in a discussion with IDN, “African leaders have to start thinking seriously about issues of healthcare or people will die. They have to realize that going abroad is no longer an option. In all, it is significant for the leaders to focus on financing sustainable public health system, make investment in the health sector using public and natural resources. Public/private partnerships have never hurt, but have to be seriously considered”.
Particularly because Africa’s population is growing, and presents future health challenges, she added. Dendere, however, stressed that various debt relief efforts by international organizations should not be an end itself, and instead African leaders must necessarily look for long-term solutions for existing pitfalls in the sector.
In the month of April, the International Monetary Fund (IMF) and the World Bank (WB) have offered debt relief to African countries. The IMF is set to provide $11 billion to 32 countries in sub-Saharan Africa that have requested assistance in fighting the coronavirus pandemic and its impact on the region’s economies.
These steps by the IMF and its partners – the World Bank, World Health Organization, the African Development Bank and the African Union – will support domestic measures including transfers to vulnerable households, monetary and fiscal policy responses, Abebe Aemro Selassie, the director of the IMF’s African Department, said in a statement.
In a similar argument, Charles Prempeh, a lecturer in Africana Studies at the African University College of Communications (AUCC), Accra and doctoral candidate at the University of Cambridge, explained in an email to IDN that there are a lot of deficiencies – ranging from poor health policies through inadequate funding of health infrastructure to training and research – that have characterized the health sector in Africa.
In his view, amid the fast spreading coronavirus in some regions, it is simply “providential” that the African continent has not recorded high numbers, compared to the western countries. But it is also true that even with the relatively smaller number of cases that most countries in Africa have recorded, they have come under disproportionate strain.
Prempreh argued that over the years, many African leaders travelled abroad (including South Africa) in search of medical care. While many African countries have research institutions, designed for studying so-called orthodox and indigenous medicines, the existence of these institutions has not yielded the expected results of enhancing the quality of healthcare on the continent, he said, adding: “In many cases, these health research institutions have been starved of funding.”
Consequently, many countries in Africa are looking up to the west to find an antidote to COVID-19 that has held the world hostage. This has implied that few Africans have invested in exploring the extent to which indigenous medicine could potentially provide an answer to the current health crisis. It is, therefore, not surprising that the COVID-19 pandemic provides lenses to peep into the deep cracks in the entire health system in Africa. It also provides important lessons for African leaders to learn now to invest in the health sector, Prempreh concluded.
Beyond all the arguments raised above, Dr Antipas Massawe, a former lecturer from the Department of Chemical and Mining Engineering, University of Dar es Salaam in Tanzania, East Africa, strongly insisted that “the scale of the challenges facing the health sector is tremendous, it requires extensive investment of resources and state to direct focus on the development agenda”.
Acknowledging that Africa is a huge continent of vast inequality where almost two-thirds still live in abject poverty and years of neglect has left the health system in tatters, Massawe added: “As compared with most of the other advanced countries that have global competitive healthcare systems, African countries spend peanuts within the budget on bolstering health infrastructure in Africa.”
The African governments should create the environment conducive for the evolution of competitive healthcare systems through prioritization. Governments have to work toward the empowerment of wealth creation endeavours, adopt system approach that would enable to understand the interdependence of African problems and outline how to tackle questions of the largely weak health as fast as possible, he suggested.
The Economic Commission for Africa (ECA), in a new report on the coronavirus pandemic, underscored that the economic implications of this disease are detrimental not only to public health systems but also the economy and sociocultural lives of the entire population of Africa.
The ECA makes explicitly clear that as the pandemic continues to impact the continent’s struggling economies whose growth are expected to slow down from 3.2 percent to 1.8 percent, within this short period it is likely to push close to 27 million people into extreme poverty.
The report launched virtually in mid-April titled, “COVID-19: Protecting African Lives and Economies” says Africa’s fragile health systems could see additional costs being imposed on them because of the growing crisis that has to-date, resulted in thousands infected Africans.
Dr Vera Songwe, UN Under-Secretary-General and Executive Secretary of ECA said: “To protect and build towards the Continent’s shared prosperity, $100 billion is needed to urgently and immediately provide fiscal space to all countries to help address the immediate safety net needs of the populations.”
Africa, notes Songwe, is particularly susceptible because 56 percent of its urban population is concentrated in slums or “informal” dwellings and only 34 percent of African households have access to basic handwashing facilities. Among others, she proposes that intellectual property on medical supplies, novel testing kits, and vaccines be shared to help Africa’s private sector play its role in the response, and most importantly policies must be firm and clear on good governance to safeguard health systems, ensure proper use of emergency funds.
In a widely circulated letter, various co-signatories in April, including 100 leading academics and writers, have called on African leaders to govern with compassion and see the current global health crisis as a chance for a radical change of direction. “Like a tectonic storm, the COVID-19 pandemic threatens to shatter the foundations of states and institutions whose profound failings have been ignored for too long. It is impossible to list these, suffice it to mention chronic under-investment in public health” in Africa notes the letter.
As a continent that is familiar with pandemic outbreaks, Africa has a head start in the management of large-scale health crises. But the belief is that “emergency” cannot and should not constitute a mode of governance. Beyond the state of emergency, however, African leaders can and should propose to their societies a new political idea of Africa, says the letter.
In consequence, it continues, the coronavirus pandemic reveals the deficit of a collective continental response, both in the health and other sectors. More than ever, we call upon leaders to ponder the necessity to adopt a concerted approach to governance sectors related to public health, fundamental research in all disciplines and to public policy.
In the same vein, health has to be conceived as essential public good, the status of health workers needs to be enhanced, hospital infrastructure needs to be upgraded to a level that allows everybody, including leaders themselves, to receive adequate treatment in Africa. Furthermore, failure to implement these reforms would be cataclysmic. For it is in the most trying moments that new/innovative orientations must be explored and lasting solutions adopted.
Today, Africa comprises 54 sovereign countries, most of which have borders that were drawn during the era of European colonialism. In the 21st century, however, the number of armed conflicts in Africa has steadily declined.
The improved stability and economic reforms have led to a great increase in foreign investment in many African nations, mainly from China, which has spurred quick economic growth in many countries, seemingly ending decades of stagnation and decline. Africa is now at risk of being in debt once again, particularly in sub-Saharan African countries.
Although it has abundant natural resources, Africa remains the world’s poorest and least-developed continent, the result of a variety of causes that may include corrupt governments and policies fraught with dubious methods. Africa is the world’s second largest and second-most populous continent after Asia. With an estimated 1.3 billion people as of 2019, it accounts for about 16% of the world’s population.
Health
Ebola: NCAA Directs Enhanced Surveillance Across Nigerian Airports
By Adedapo Adesanya
The Nigeria Civil Aviation Authority (NCAA) has directed airlines, airport operators and other aviation stakeholders to intensify public health surveillance measures following the outbreak of Ebola Virus Disease (EVD) in parts of the Democratic Republic of Congo (DRC) and Uganda.
In a circular dated May 18, 2026, the NCAA said the directive became necessary due to growing concerns over the spread of the disease and the critical role of the aviation sector in preventing cross-border transmission.
The authority noted that although no confirmed case linked to the outbreak has been recorded in Nigeria, it is collaborating with the Federal Ministry of Health, the Nigeria Centre for Disease Control (NCDC), Port Health Services and international health organisations to closely monitor the situation.
According to the NCAA, health authorities in the DRC recently identified a cluster of severe illnesses among healthcare workers in the Bunia Health Zone in the northeastern part of the country.
Recall that Nigeria also said it would tighten surveillance after the World Health Organisation (WHO) declared a public health emergency after Ebola killed over 80 people in Congo and Uganda.
Laboratory investigations later confirmed the presence of the Bundibugyo virus, a strain of the Ebola virus family known to cause severe viral haemorrhagic disease in humans.
The authority stated that there is currently no licensed vaccine specifically approved for the Bundibugyo strain, while treatment remains largely supportive and symptom-based.
The NCAA listed symptoms associated with Ebola Virus Disease to include sudden fever, severe fatigue, persistent headache, vomiting, abdominal pain and bleeding manifestations such as nosebleeds or vomiting blood.
It stressed that early detection and immediate reporting remain critical to preventing the international spread of the disease.
As part of preventive measures, the authority said disease surveillance systems at airports have been strengthened, while contact tracing, case reporting mechanisms and border health screening procedures are also being reinforced.
The NCAA further directed pilots to notify Air Traffic Control of any suspected communicable disease cases onboard aircraft, in line with the Nigeria Civil Aviation Regulations.
It also instructed flight crew members to complete and submit Aircraft General Declaration forms for all suspected cases and mandated airlines to ensure passenger locator forms are completed and handed over to Port Health Services upon arrival.
The authority added that airlines must ensure aircraft are properly equipped with first aid kits, universal precaution kits and emergency medical kits.
It also urged operators to reinforce crew training on the identification and management of communicable diseases and ensure strict adherence to infection prevention and control guidelines.
The NCAA called on all aviation stakeholders to remain vigilant and comply fully with established public health protocols to safeguard passengers, crew members and the general public from potential health threats.
Health
Nigeria on High Alert as WHO Declares Ebola Emergency of International Concern
By Adedapo Adesanya
The Nigeria Centre for Disease Control and Prevention (NCDC) has said that although the country currently has no confirmed case of Ebola Virus Disease (EVD), it is, nevertheless, actively strengthening surveillance.
This comes as the World Health Organisation (WHO) declared the Ebola outbreak in Congo and Uganda a public health emergency of international concern, after 80 deaths were attributed to the disease.
The WHO, however, stopped short of declaring a pandemic, saying it did not meet the necessary criteria. The United Nations agency advised countries against closing borders or restricting trade.
Early symptoms include fever, muscle pain, fatigue, headache, and sore throat, and are followed by vomiting, diarrhoea, a rash, and bleeding.
In a statement by its Director General, Mr Jide Idris, on Sunday, the NCDC noted that it is also ramping up laboratory readiness, infection prevention, and public awareness efforts across the country.
He said the centre was closely monitoring the situation due to increasing regional movement across African countries and was working with relevant stakeholders, including the Port Health Services under the Federal Ministry of Health and Social Welfare, to strengthen preparedness within Nigeria’s public health system.
“NCDC is closely monitoring the situation and working with relevant stakeholders, including the Port Health Services, to ensure continued vigilance and preparedness within the public health system,” he stated.
The NCDC boss described Ebola virus disease as a severe viral illness transmitted through direct contact with the blood, bodily fluids, secretions, or contaminated materials of infected persons or animals.
He noted that the disease has an incubation period ranging from two to 21 days, while symptoms include fever, weakness, headache, muscle pain, sore throat, vomiting, diarrhoea, and, in severe cases, unexplained bleeding.
Recall that Nigeria gained international recognition for successfully containing an Ebola outbreak in 2014 after an infected traveller arrived in Lagos from Liberia.
Healthcare workers were advised to maintain a high index of suspicion for Ebola, especially in patients presenting symptoms compatible with the disease alongside relevant travel or exposure history.
Idris stressed the importance of strict adherence to infection prevention and control measures, including early identification and isolation of suspected cases, proper use of personal protective equipment, hand hygiene, and prompt reporting through established channels.
“NCDC will continue to monitor the situation closely and provide updates as necessary,” he added.
NCDC advised Nigerians to remain calm, maintain good hand hygiene, avoid misinformation, and report unusual illnesses promptly.
Health
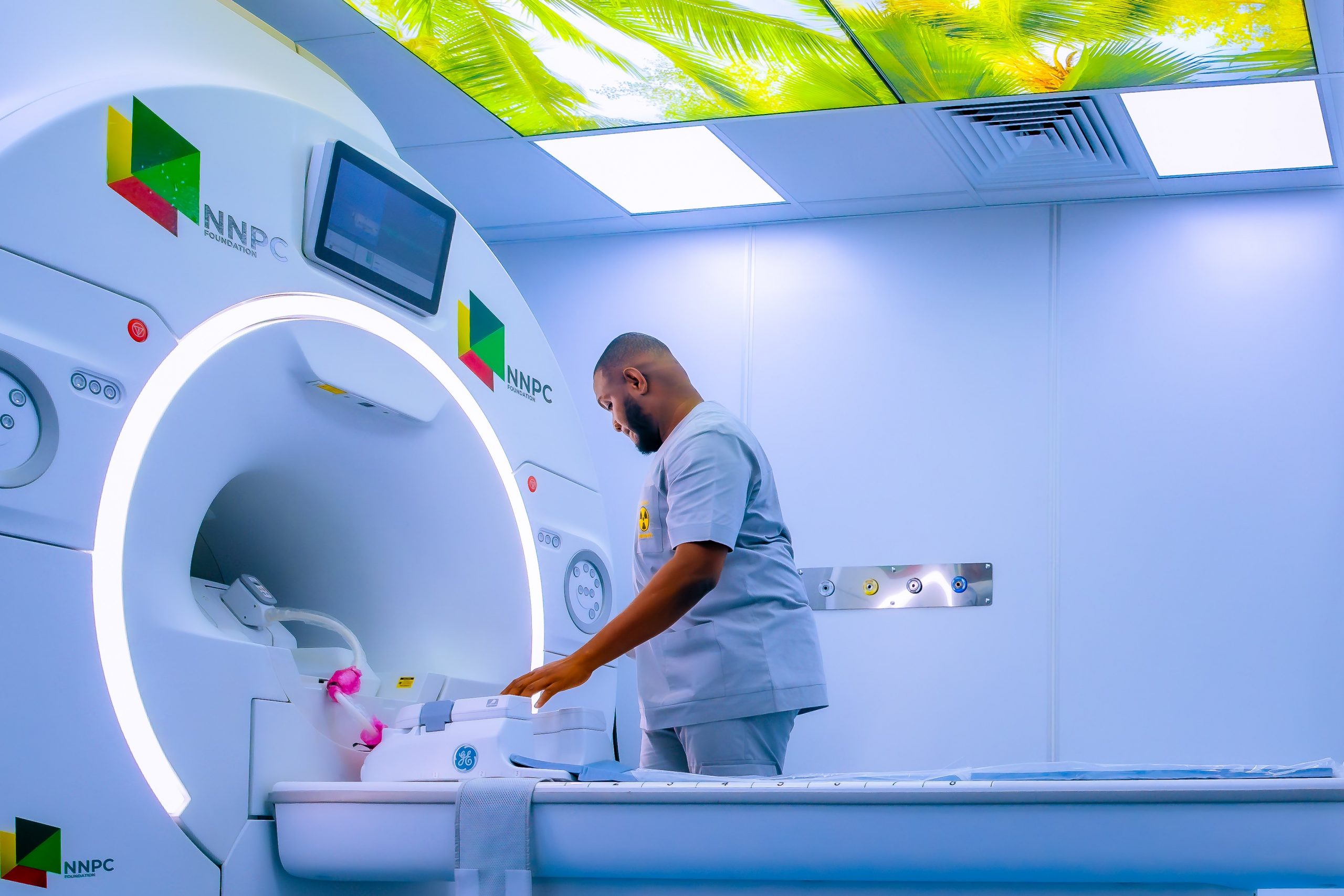
NNPC Donates MRI Machine, Others to Nnewi Teaching Hospital
By Modupe Gbadeyanka
A 1.5 Tesla Magnetic Resonance Imaging (MRI) machine has been donated to the Nnamdi Azikiwe University Teaching Hospital (NAUTH), Nnewi, Anambra State, by the corporate social responsibility arm of the Nigerian National Petroleum Company (NNPC) Limited, NNPC Foundation.
In a statement on Sunday by its Chief Corporate Communications Officer, Mr Andy Odeh, the state-owned oil organisation said the medical item was given to the healthcare institution as part of its commitment to improving healthcare access and strengthening medical infrastructure across Nigeria.
The MRI system is expected to significantly improve access to advanced diagnostic imaging services for millions of Nigerians across the South-East (Anambra, Enugu, Imo, Abia and Ebonyi States) as well as neighbouring Delta State.
The foundation also provided critical supporting infrastructure, including RF shielding systems, chillers, backup UPS systems, electrical installations, specialised imaging accessories, ventilation systems, CCTV and oxygen monitoring systems, intercom communication facilities, and other patient comfort technologies designed to ensure optimal operation of the facility.
Before now, patients requiring advanced MRI diagnostic services often faced prolonged waiting periods, exorbitant costs, and the burden of travelling long distances in search of functional imaging centres.
But it is believed that the intervention of the NNPC Foundation would provide succour to patients.
At the presentation of the items to the institution over the weekend, the chief executive of the NNPC, Mr Bashir Bayo Ojulari, represented by the Managing Director of NNPC Foundation, Mrs Emmanuella Arukwe, described the intervention as a strategic investment in healthcare access, diagnostic precision, and improved patient outcomes, noting that the facility aligns with the company’s commitment to building sustainable systems and impactful national institutions.
“The installation of the MRI in NAUTH exemplifies our commitment, as our intent is to build enduring institutions, sustainable systems and legacies. This intervention aligns with our conviction that access to quality healthcare underpins human dignity, longevity and economic productivity,” Mr Ojulari stated.
He described the company’s social investments as viable currencies that strengthen the relationship between the Company’s core mandate of providing and managing energy for Nigerians and meeting stakeholders’ expectations.
In his remarks, the Governor of Anambra State, Mr Charles Soludo, who was represented by the Commissioner for Health, Dr Afam Obidike, said the intervention would enhance safe and precise diagnosis and treatment for patients across the South-East region.
He also commended NNPC Foundation for donating the MRI facility to the state, noting that the intervention would significantly improve access to quality healthcare services for the people.
The Chief Medical Director of NAUTH, Prof Joseph Ugboaja, thanked the donor for the items, saying NNPC Foundation has demonstrated that corporate social responsibility is not just a policy statement but a lifeline for institutions like ours.
“For too long, patients in our catchment area have had to travel long distances to access this level of diagnostic precision, often at prohibitive costs. With this installation, we will eliminate that burden,” he enthused.
-

 Feature/OPED6 years ago
Feature/OPED6 years agoDavos was Different this year
-
Travel/Tourism10 years ago
Lagos Seals Western Lodge Hotel In Ikorodu
-

 Showbiz3 years ago
Showbiz3 years agoEstranged Lover Releases Videos of Empress Njamah Bathing
-

 Banking8 years ago
Banking8 years agoSort Codes of GTBank Branches in Nigeria
-

 Economy3 years ago
Economy3 years agoSubsidy Removal: CNG at N130 Per Litre Cheaper Than Petrol—IPMAN
-

 Banking3 years ago
Banking3 years agoSort Codes of UBA Branches in Nigeria
-

 Banking3 years ago
Banking3 years agoFirst Bank Announces Planned Downtime
-

 Sports3 years ago
Sports3 years agoHighest Paid Nigerian Footballer – How Much Do Nigerian Footballers Earn

