Health
WHO Partners Health Authorities to Bolster Monkeypox Testing in Africa
By Adedapo Adesanya
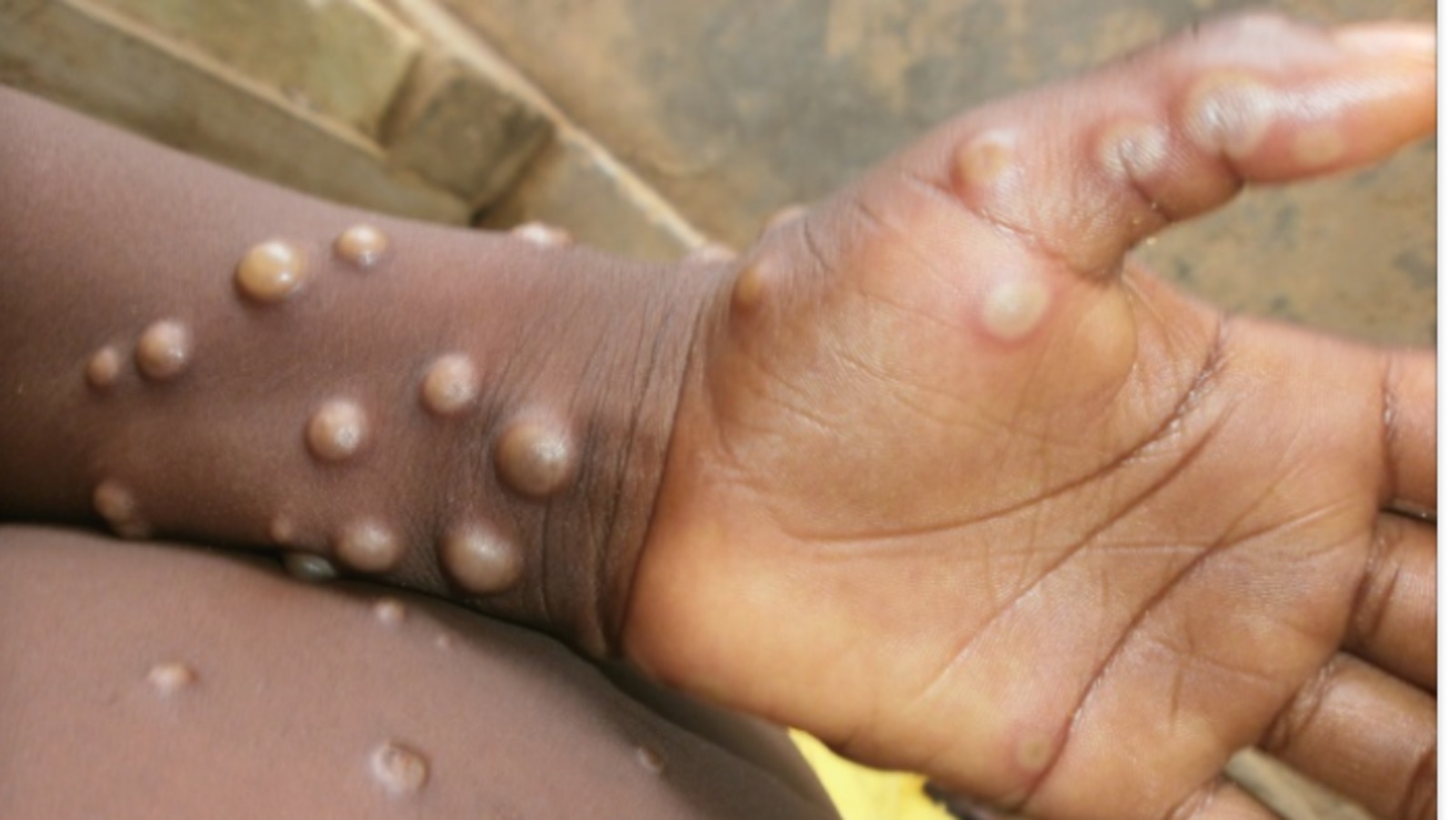
The World Health Organisation (WHO) has announced that it was working with national health authorities in Africa to bolster surveillance and laboratory diagnosis to detect cases and deter a silent spread of the virus.
The continent as of June 28 has reported 1,821 cases in 13 countries of which 109 are laboratory confirmed in nine countries. The number of confirmed cases accounts for 2 per cent of the more than 4,500 confirmed cases globally.
However, there are a large number of suspected cases in the region, 81 per cent of which are in the Democratic Republic of the Congo, underlining the need for increased diagnostic capacity.
While all African countries have the polymerase chain reaction machines needed to test for monkeypox thanks to reinforced laboratory capacity in the wake of COVID-19, many lack reagents and in some cases training in specimen collection, handling and testing.
As a result, WHO is working to secure 60,000 tests for Africa, with around 2,000 tests and reagents to be shipped to high-risk countries and 1,000 to those facing lower risk.
Over the past months, five more African countries have received donations of reagents from partners, bringing to 12 the number of countries in the region with enhanced monkeypox diagnostic capacity. Another group of countries in West Africa will receive reagents after participating in a training.
Outside the six countries in Africa with a history of human transmission, monkeypox has also been reported in three countries which have not previously had any human cases. These include Ghana, Morocco and South Africa, which have confirmed the disease in two patients with no travel history, suggesting there is a high possibility of local transmission.
“The geographic spread of monkeypox to parts of Africa where cases have never been detected before is a worrying sign,” said Dr Matshidiso Moeti, WHO Regional Director for Africa. “It is critical that we support national efforts to boost surveillance and laboratory diagnosis, which are the cornerstones of disease control.”
To deepen the analysis of monkeypox transmission patterns, WHO is supporting countries to capitalize on the improved genomic sequencing capacity built during the COVID-19 pandemic.
Many years of research have led to the development of new and safer (second- and third-generation) vaccines for smallpox, some of which may be useful for monkeypox and one of which (MVA-BN) has been approved for the prevention of monkeypox. However, supplies are limited.
“What happened in the early days of the COVID-19 vaccine rollout when Africa watched on the sidelines as other countries snapped up limited supplies must not be allowed to recur. There are some signs that this is already happening,” said Dr Moeti. “The current global spotlight on monkeypox should be a catalyst to beat this disease once and for all in Africa. For this, we know vaccines are a critical tool.”
WHO is also working closely with the Member States and partners to define what type of coordination mechanism could be put in place to ensure fair access to vaccines. There are many regulatory, legal, operational, technical, and other issues to clarify before an allocation mechanism is fully operational.
With limited vaccines and antivirals, WHO does not recommend mass vaccination for monkeypox but rather targeted vaccination for people who have been exposed or are at high risk including health workers, laboratory personnel and outbreak team responders.
Health
WHX in Lagos 2026: Nigeria Open for Healthcare Investment—FG

By Modupe Gbadeyanka
The federal government has urged global investors and innovators to tap into the Nigerian healthcare ecosystem, which is projected to grow by 7.1 per cent, reaching a market value of $161.7 million by 2027.
This advice was given by the Minister of State for Health and Social Welfare, Mr Isiaq Salako, at the opening of the World Health Expo (WHX in Lagos 2026), formerly known as Medic West Africa, on Tuesday in Lagos.
The broader West African market is expected to reach more than $11 billion, providing investors with an opportunity to get a good return on investment.
“Nigeria is open for healthcare investment. We want platforms like WHX in Lagos to serve as a critical conduit for translating this investment ambition into tangible technology access for our hospitals and patients,” the Minister, who declared the event open on behalf of President Bola Tinubu, said.
He praised the organisers of the expo, which welcomed over 8,000 healthcare professionals and 500 exhibitors spanning 40 countries, for growing the programme into a vital catalyst for West African healthcare transformation.
Addressing the stark reality that between 85 per cent and 99 per cent of medical equipment and in vitro diagnostics in West Africa are currently imported, Mr Salako outlined aggressive federal interventions designed to dismantle supply chain vulnerabilities and skyrocket local manufacturing capabilities.
He also spotlighted key presidential directives, including the Presidential Initiative to Unlock Healthcare Value Chains (PVAC) and the Presidential Executive Order for the Pharmaceutical and Allied Sectors, both engineered to catalyse health security, drive economic growth, and generate employment through strategic private-sector collaborations and Public-Private Partnerships (PPPs).
“Our commitment to improving access to modern equipment and technologies in hospitals is backed by concrete action. The government has inaugurated the $1.2 billion Sector-Wide Approach (SWAP) initiative, a comprehensive overhaul addressing financing, workforce development, and infrastructure.
“Furthermore, for the 2025 fiscal year, the Federal Government committed N402 billion specifically for health sector infrastructure investment,” he stated, also highlighting an expansive health infrastructure upgrade program in partnership with the Nigeria Sovereign Investment Authority (NSIA).
According to him, this phased initiative is actively delivering oncology and nuclear medicine centres across six tertiary hospitals, alongside establishing 22 modern medical diagnostic centres, seven cardiac catheterisation laboratories, and expanded radiology and clinical pathology capabilities distributed across Nigeria’s six geopolitical zones.
Also speaking, the chief executive of EHA Clinics, Dr Ifunanya Ilodibe, stressed the urgent need to support and unify fragmented growth within the healthcare system, noting that WHX serves as the precise ecosystem platform required to bring together policymakers, clinicians, and investors to move actionable strategies forward.
Also, the President of the Healthcare Federation of Nigeria (HFN) and Country Director of PharmAccess, Njide Ndili, said, “HFN bridges the gaps in health financing, opening up critical connections to achieve true health sovereignty,” praising Africa CDC’s historical intervention, particularly during the Ebola crisis and urged participants to utilise the WHX exhibition floor to forge collaborations capable of scaling locally produced medical equipment.
The Lagos State Commissioner for Health, Mr Akin Abayomi, on his part, highlighted the enforcement of the National Health Insurance Authority (NHIA) Act in Lagos State as a landmark regulatory milestone. The Act mandates health insurance for all residents, structuring the financial environment to guarantee medical protection across various socioeconomic levels.
Delivering the keynote address, the Special Regional Representative of the Director General of the Africa CDC Western Regional Coordinating Centre, Prof. Aliko Ahmed, called on leaders in geopolitical positions to enact liberating trade policies aligned with the African Continental Free Trade Area (AfCFTA) to shape the continental agenda, emphasising that the Africa CDC will fiercely prioritise building trust in locally manufactured healthcare products.
WHX in Lagos 2026 runs for three days, featuring accredited forums, cutting-edge product showcases, and high-level networking tracks designed to translate billions in public and private investment into immediate technology access for hospitals and patients.
Health
Euracare Secures Court Order Halting Inquest into Chimamanda Son’s Death

By Adedapo Adesanya
The coroner’s inquest into the death of 21-month-old Nkanu Adichie-Esege, son of renowned author Chimamanda Ngozi Adichie, suffered a major setback on Wednesday after Euracare Multi-Specialist Hospital informed the coroner’s court that it had obtained an order of the Lagos State High Court staying further proceedings in the probe.
The matter came before Coroner Magistrate Atinuke Adetunji at Court 9, Igbosere Magisterial District, Yaba, Lagos, and was scheduled for the commencement of witness’ testimony.
Counsel to Euracare Multi-Specialist Hospital, Professor Taiwo Osipitan (SAN), told the court that the hospital had initiated judicial review proceedings challenging, among other issues, the jurisdiction of the Coroner’s Court to conduct the inquest in the absence of the deceased’s body.
He disclosed that the High Court had granted leave for the judicial review application and ordered that the leave operate as a stay of proceedings pending the determination of the suit.
The senior advocate also informed the court that although the Lagos State Attorney-General’s Office denied seeing the originating processes from the High Court, proof of service was available.
Responding on behalf of the family, Mr Kemi Pinheiro (SAN) confirmed receipt of both the originating processes and the High Court order.
While acknowledging the obligation of all parties to comply with court orders, he informed the coroner that the family had already filed four witness statements on oath, including that of Dr Ivara Esege, as well as statements from independent medical experts from Nigeria and the United States, who are expected to testify at the inquest.
Mr Pinheiro urged the court not to adjourn the matter indefinitely, but to a definite date after the court vacation to enable parties to report on developments in the High Court proceedings.
He also highlighted the need for transparency and public confidence in the fact-finding process, saying, “He who is innocent does not fear an open inquest.”
Counsel representing Atlantis Paediatric Hospital supported the request for a definite adjournment rather than an indefinite postponement.
Following submissions by counsel, the Coroner adjourned the matter until October 8, 2026, for a report on the status of the High Court proceedings.
Health
Gavi Promises $50m for Bundibugyo Ebolavirus Vaccines

By Modupe Gbadeyanka
About $50 million has been promised by Gavi, the Vaccine Alliance, through its First Response Fund (FRF), to support the response to the ongoing Bundibugyo ebolavirus outbreak.
A statement from the organisation made available to Business Post on Monday said up to $40 million would be available to enable accelerated access to investigational doses and, eventually, approved vaccines, while a further $10 million would support outbreak response and protection of routine immunisation services in impacted countries.
“We need to act now to ensure that, once one or more vaccine candidates are ready, manufacturers are in a position to start producing doses at scale,” the chief executive of Gavi, Dr Sania Nishtar, was quoted as saying.
“Leveraging this allocation, Gavi will work closely with CEPI and partners to design the right incentives to achieve this goal, exploring all options, including potential Advance Purchase Commitments.
“This effort, alongside ensuring emergency funds are on hand to support outbreak response and protect routine immunisation services in the communities impacted, is exactly what our First Response Fund was designed for,” Dr Nishtar added.
The First Response Fund is the only globally approved mechanism that allows “at-risk” financing for scaled-up production of vaccines under development. This means Gavi is able to make vital early investments even when development outcomes are uncertain.
The $40 million in immediate surge financing that has been approved today will enable manufacturers of the leading candidates of a vaccine against the Bundibugyo virus to directly commit to high-capacity manufacturing.
This, in turn, will ensure that, as soon as clinical trials demonstrate positive outcomes, investigational vaccine doses could be deployed rapidly to support outbreak response.
Looking to the longer-term, Gavi will also provide incentives for manufacturers to adopt the fastest pathways towards WHO Emergency Use Listing (EUL) and/or WHO Prequalification (PQ), which are critical global approvals that will enable the rapid use of these vaccines in future emergencies.
In the coming weeks, Gavi will finalise the design of a financial mechanism that leverages the $40 million FRF allocation to achieve these vaccine access goals, in close partnership with the Coalition for Epidemic Preparedness Innovations (CEPI) as well as WHO, Africa Centres for Disease Control and Prevention (Africa CDC) and UNICEF.
The final design will take into account the characteristics of individual vaccine candidates and the needs of their manufacturers and may include mechanisms such as Advance Purchase Commitments. Work will also be undertaken to ensure successful candidates from African-based vaccine manufacturers can benefit from accelerated support through Gavi’s African Vaccine Manufacturing Accelerator (AVMA) initiative.
In addition to these investments, Gavi will also immediately release US$ 10 million to support countries and partners with outbreak response.
This funding will support implementation of national outbreak response plans, including targeted investments to protect routine immunisation, protect health care workers and ensure readiness for future vaccines. Gavi will work closely with countries, partners including Africa CDC, WHO, UNICEF, World Bank, and donors to ensure these investments complement other efforts.
-

 Feature/OPED6 years ago
Feature/OPED6 years agoDavos was Different this year
-
Travel/Tourism10 years ago
Lagos Seals Western Lodge Hotel In Ikorodu
-

 Showbiz3 years ago
Showbiz3 years agoEstranged Lover Releases Videos of Empress Njamah Bathing
-

 Banking8 years ago
Banking8 years agoSort Codes of GTBank Branches in Nigeria
-

 Economy3 years ago
Economy3 years agoSubsidy Removal: CNG at N130 Per Litre Cheaper Than Petrol—IPMAN
-

 Banking3 years ago
Banking3 years agoSort Codes of UBA Branches in Nigeria
-

 Banking3 years ago
Banking3 years agoFirst Bank Announces Planned Downtime
-

 Sports3 years ago
Sports3 years agoHighest Paid Nigerian Footballer – How Much Do Nigerian Footballers Earn

